AI system identifies patients who will be at risk within 48 hours

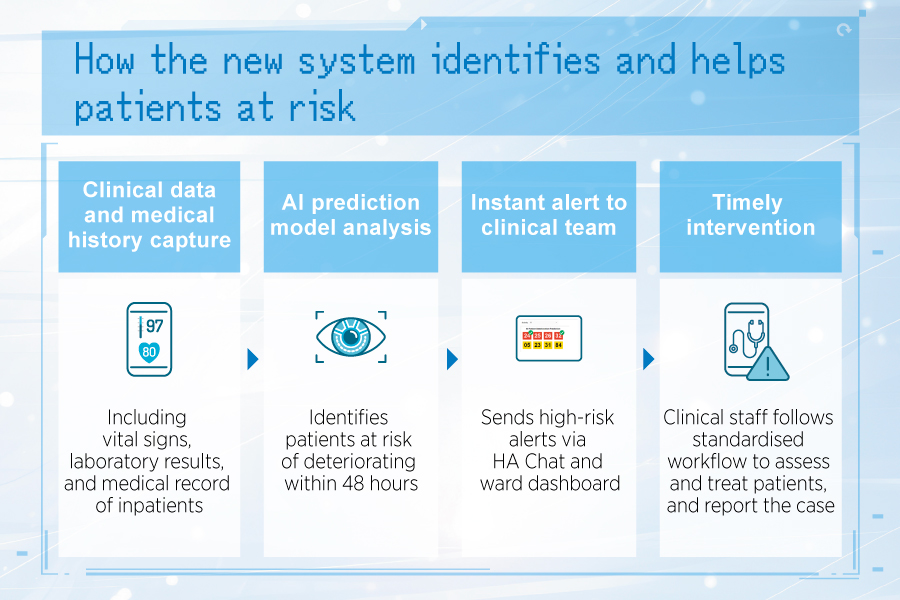
Patient deterioration often occurs swiftly and without warning. If early signs can be identified, timely intervention can be provided. The Hospital Authority (HA) has introduced an Artificial Intelligence (AI) Patient Deterioration Prediction System, which uses AI to analyse three sets of data — vital signs, laboratory results, and clinical records — with a total of more than 20 data items. The system predicts the likelihood of deterioration of inpatients within 48 hours. If a high-risk case is identified, the system will send an instant alert message via HA Chat and update the ward dashboard to notify clinical staff.
Detected the abnormality of an asthma patient and allowed early intervention
Pok Oi Hospital (POH) is currently piloting the system to all inpatient wards. New Territories West Cluster Coordinator (Information Technology/Information Systems) Dr Lui Chun-tat recalls an asthma patient who was initially in stable condition, and the system recognised an increase in patient's respiratory rate from a baseline of 12 to 14 breaths per minute to 20, while there is tachycardiac response to near 120 per minute. Alongside other clinical parameters, the system issued a high-risk alert. Nurse informed on-duty doctor after stabilisation. The attending doctor prescribed bronchodilators to relieve the patient's condition, and mitigated the risk of further deterioration to intubation and ventilation. Dr Lui regards the system as a clinical safety net that anticipates subtle changes before major deterioration occurs, such as loss of consciousness or abrupt drop in blood pressure.
To adapt to its implementation, POH IT team had worked together with the Quality & Safety Division to introduce a standardised clinical response framework called the Smart-CARES Bundle, which provides clear assessment and escalation guidelines for frontline healthcare staff. POH Advanced Practice Nurse Lau Man-chung says when frontline staff receives alerts through HA Chat and the ward dashboard, they will acknowledge the alert, immediately assess the patient's condition and measure his vital signs in accordance with the step-by-step standardised care protocol. If an airway obstruction is detected, for instance, suction and oxygen therapy will immediately be given and the case will be escalated to doctor. The Smart-CARES Bundle also provides standardised framework of assessment and treatment for interns and doctors with less experience.
Chief Manager (Health Informatics) Dr Joyce Chan Ka-yin explains that the system analyses more than 20 data items, including blood pressure, blood oxygen level, pulse, and patient medical history. It automatically calculates the patient's latest risk level. The system offers significantly higher accuracy compared with the Modified Early Warning Score (MEWS) system previously used and has a prediction accuracy of up to 92% and a false positive rate of only around 1%.

The system not only identifies high-risk patients but also displays potential causes of deterioration to support more precise clinical decision-making. It will be extended to more public hospitals in the future to further improve the quality of healthcare services, Dr Chan says.